An Occupational Therapist's primary goal is to increase a patient’s capacity to engage in everyday activities they need or want to do. Sometimes, customized devices and materials (such as splints) are used to gently shape and guide a patient’s extremities to assist with engaging in these everyday activities. Collette Edge and Christy Gould, Occupational Therapists at Pullman Regional’s Summit Therapy & Health Services, explain what splinting is, how it relates to occupational therapy, and what the splinting process looks like.
What is splinting?
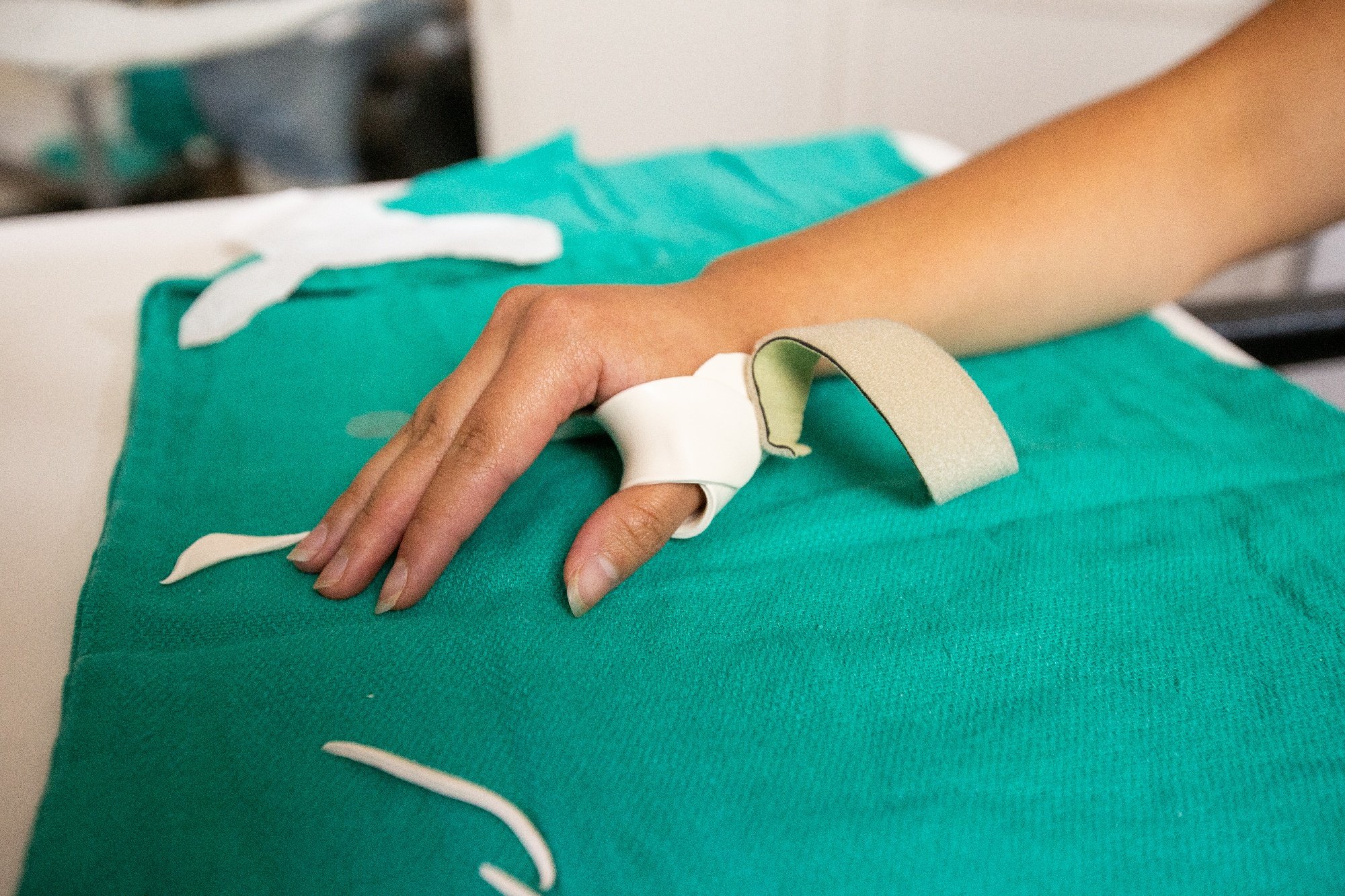
Splinting is the use of thermoplastic material (starts hard, gets soft in warm water for custom molding, and then hardens again as it cools) to hold a person’s arm, hand, or finger in a specific position. Occupational Therapists are trained to design and create custom splints to address a wide spectrum of joint disorders. Splinting material comes in different thicknesses, colors, and either smooth or perforated for better air flow. Velcro and straps are often used to secure the thermoplastic mold around the joint(s) and allow the patient to adjust the fit for comfort.
There are generally two types of splints customized at Summit Therapy & Health Services that allow for specific degrees of movement to the targeted joint:
- Static splinting immobilizes a joint/joints so that healing can occur in the bones or tissues with little-to-no movement.
- Dynamic splints are used to allow movement at some joints while restricting movement at others of the same arm, wrist, or hand. Dynamic splints may include hinges, strings, and slings.
In addition to custom splinting, occupational therapists use neoprene splints (elastic material) for joint support when the motion of the joint is not in need of being restricted, but the joint needs gentle support.
What does the splinting process entail?
The process of creating a splint includes a hot water bath, heat gun, plastic molding material, neoprene straps, Velcro, suture removal kits and Coban wound wrap.
When patients are getting fitted for a splint, they sit at a table across from their occupational therapist, who traces their hand on a paper towel (think Thanksgiving hand turkey craft project)! This cutout is then transferred to a sheet of thermoplastic material to shape the custom splint.
What does splinting do?
When a joint has too little or too much range of motion due to acute injury (bone fracture, tendon rupture, burn, traumatic brain injury, or neurological conditions) or chronic joint deformity (arthritis, repetitive use injury, neurological conditions), a splint can help reduce/increase mobility, support healing and increase the use of the upper extremity in everyday tasks. When a splint is used to hold a body part/joint in a specific position to promote healing or to promote good alignment, it is called an “antideformity” position splint.
Additionally, splinting can be utilized to increase the range of motion around a joint when the soft tissue has been shortened and prevents the joint from moving. This is often due to spasticity (strong, sustained muscle contraction), burn, or scarring. A splint is then created to stretch the soft tissue in graded lengths over time. It prevents deformity of that body part by helping it heal correctly or by holding that part in a good position while other body parts move during functional activities.
Who is a good candidate for a splint?
Some of the more common ailments that use splints as part of the rehabilitation process include carpal tunnel syndrome, trigger finger, tendonitis of the fingers or wrist, stroke, multiple sclerosis, bone fractures, and burns.
Patients are commonly referred to an occupational therapist by a surgeon or primary care physician and prescribed a specific type of splint; these splints follow a specific ‘Rehabilitation Protocol.’ Splinting protocols direct the frequency, duration, and progression of splint use which can vary between constant (24 hours), nighttime, intermittently during the day, or for task-specific performance. These protocols help guide the occupational therapist and patient through safe, research-based outcome measures for rehabilitation. Protocols are designed to allow the maximum amount of movement that is considered safe for the injured body part, based on the patient’s specific diagnosis and/or surgical procedure(s).